Periodontal Disease: Causes, Symptoms, Treatment, and Prevention
Periodontal disease—commonly known as gum disease—is an infection and inflammation of the gums and the supporting bone around your teeth. It starts quietly, often without pain, but left untreated, it can damage the structures that hold your teeth in place and eventually lead to tooth loss.
Healthy gums do more than just look good. They form a tight seal around each tooth, protecting the underlying bone and periodontal ligament from bacteria. This support system keeps teeth stable for everyday functions like chewing food, speaking clearly, and smiling with confidence. When gum tissue breaks down, these basic activities become compromised.
Here’s the reality: gum disease is one of the most common oral health conditions in adults worldwide. According to data from the National Institute of Dental and Craniofacial Research, roughly 42% of U.S. adults aged 30 and older have some form of periodontitis. The good news? Most cases are preventable with good oral hygiene and regular dental visits.
The condition exists on a spectrum. Gingivitis represents the mildest form—gums become red and swollen, and you might notice bleeding gums when brushing. At this early stage, damage is reversible. Periodontitis, however, involves deeper infection and bone loss that’s much harder to reverse. Understanding this distinction matters because catching problems in the early stages makes treatment far more effective.
This article covers what periodontal disease actually is, its causes and risk factors, warning signs to watch for, how the disease progresses through stages, treatment options ranging from nonsurgical treatment to surgical procedures, prevention strategies, and the connection between gum health and overall health. If you notice red, swollen, or bleeding gums, or persistent bad breath that doesn’t improve with brushing, prompt professional evaluation is advised.
What Is Periodontal Disease?
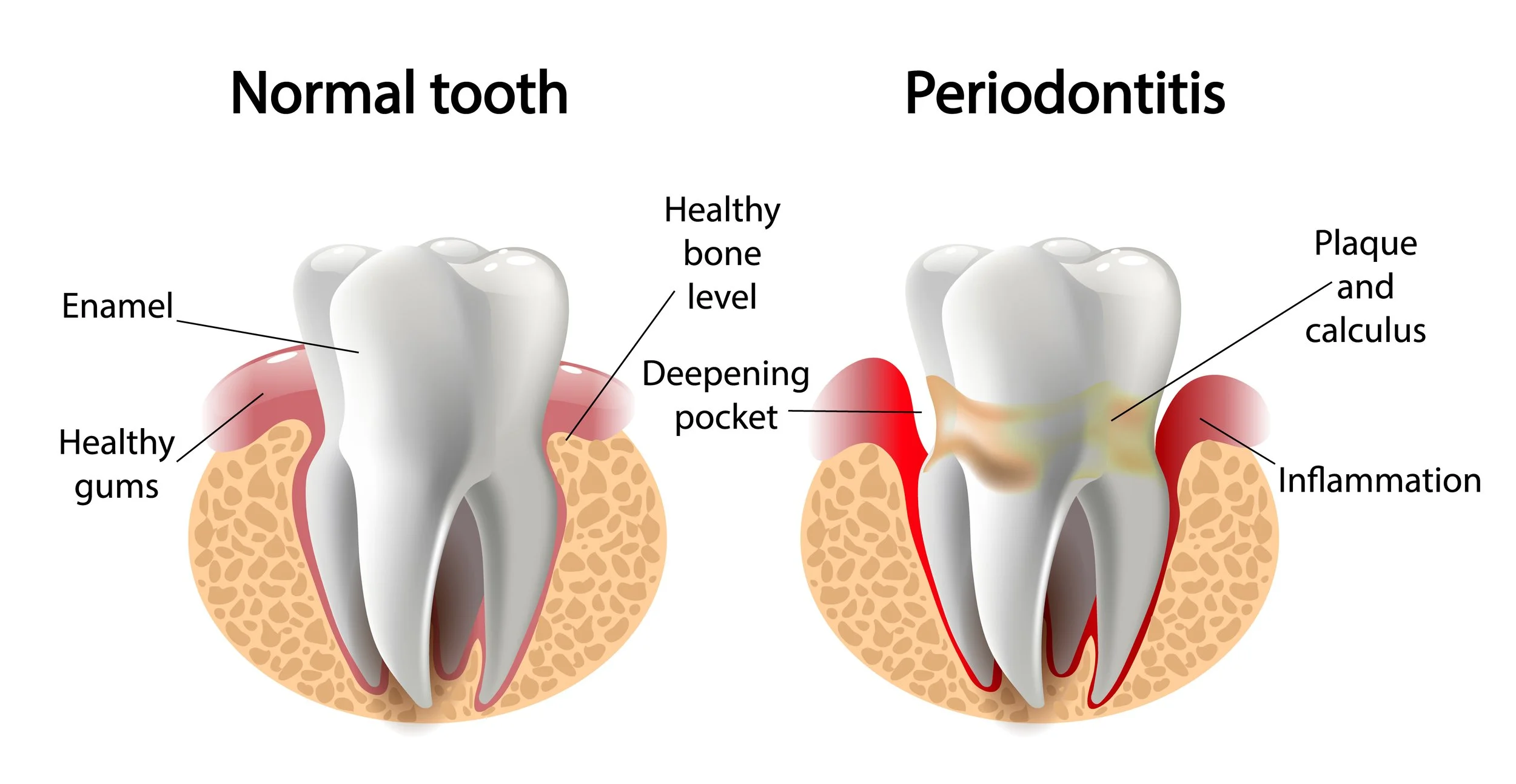
Periodontal disease refers to a spectrum of conditions affecting the periodontium—the structures that surround and support your teeth. This includes the gums, the periodontal ligament (fibers connecting teeth to bone), the cementum covering tooth roots, and the underlying bone of the jaw.
Gingivitis vs. Periodontitis
Gingivitis is the earliest stage of gum disease. It affects only the soft tissue of the gums, causing redness, swelling, and bleeding when you brush or floss. Crucially, no bone loss has occurred yet, and the condition is fully reversible with proper dental care.
Periodontitis develops when gingivitis goes untreated. Bacteria extend below the gumline, triggering a chronic inflammatory response. Your immune system releases substances meant to fight infection, but these same substances—along with bacterial toxins—gradually destroy the supporting bone and periodontal ligament. This creates periodontal pockets, spaces between teeth and gums where plaque and tartar accumulate beyond the reach of your toothbrush.
How It Develops
The process starts with plaque buildup. Dental plaque is a sticky bacterial film that forms on tooth surfaces every day. If not removed through daily brushing and flossing, plaque hardens into tartar (also called calculus) within 24-72 hours. Tartar buildup, especially below the gumline, creates an environment where harmful bacteria thrive.
Key periodontal pathogens include Porphyromonas gingivalis, Tannerella forsythia, and Treponema denticola. These bacteria and their metabolic byproducts activate an inflammatory cascade involving immune cells, cytokines, and enzymes that break down tissue and stimulate bone resorption.
Why Early Detection Matters
Once bone and attachment around teeth are lost, they typically cannot be fully restored. This makes early detection critical. The challenge? Many people experience no pain during the early and moderate stages of periodontal gum disease. Symptoms may be limited to occasional bleeding or bad breath—easy to dismiss or ignore.
This is why regular dental checkups matter even when your gums “feel fine.” Your dentist or dental hygienist uses a tiny ruler called a periodontal probe to measure pocket depths around each tooth, along with X-rays to assess bone levels. These examinations catch disease before it progresses to irreversible damage.
Common Causes and Risk Factors of Periodontal Disease
Periodontal disease develops from an interaction between bacterial plaque and individual risk factors. It’s not simply about “poor brushing”—your genetics, health conditions, and lifestyle all influence whether plaque triggers destructive inflammation.
Poor Oral Hygiene
Infrequent brushing, skipping flossing, and avoiding professional cleanings allow plaque to accumulate along and below the gumline. Without regular removal, plaque hardens into tartar that you cannot remove at home. This creates the conditions for dysbiosis—a shift toward more harmful bacteria in your mouth.
Tobacco Use
Smoking and all forms of tobacco represent major risk factors for periodontitis. Research consistently shows that smokers have:
Higher prevalence and severity of gum disease
Slower healing after treatment
Poorer response to periodontal therapy
Risk that persists for years after quitting (though it does diminish over time)
Genetics and Family History
Some people are simply more susceptible to periodontal disease due to inherited traits. Variations in genes controlling immune response—particularly those affecting inflammatory mediators like IL-1—influence how aggressively your body reacts to bacterial plaque. If your parents or siblings have had significant gum problems, you may share this susceptibility.
Systemic Health Conditions
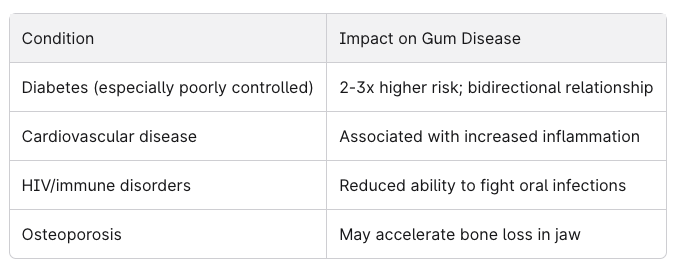
Certain health conditions substantially increase periodontal risk:
The diabetes connection deserves special attention. Poor glycemic control increases susceptibility to infection, while untreated periodontal disease can make blood sugar harder to manage. According to the American Dental Association, this two-way relationship makes dental care essential for diabetes management.
Hormonal Changes
Puberty, pregnancy, menstrual cycles, and menopause can all affect gum health. Hormonal changes increase blood flow to gum tissue and alter how the immune system responds to plaque, making gums more prone to inflammation even with the same amount of bacteria present.
Medications and Dry Mouth
Many common medications reduce saliva flow, including certain medicines for depression, high blood pressure, and allergies. Saliva plays a crucial cleansing role in the mouth. Without adequate saliva, plaque accumulates more readily, and poor nutrition of oral tissues follows.
Additional Risk Factors
Stress (weakens immune response)
Diet high in sugar and refined carbohydrates
Mouth breathing
Misaligned or crowded teeth that are hard to clean
Poor nutrition, especially deficiencies in vitamins C and D
Signs and Symptoms of Gum Disease
Gum disease can progress silently for months or years. However, there are warning signs you can watch for at home—catching them early gives you the best chance of reversing damage.
Early Warning Signs
The most common gum disease symptoms in early stages include:
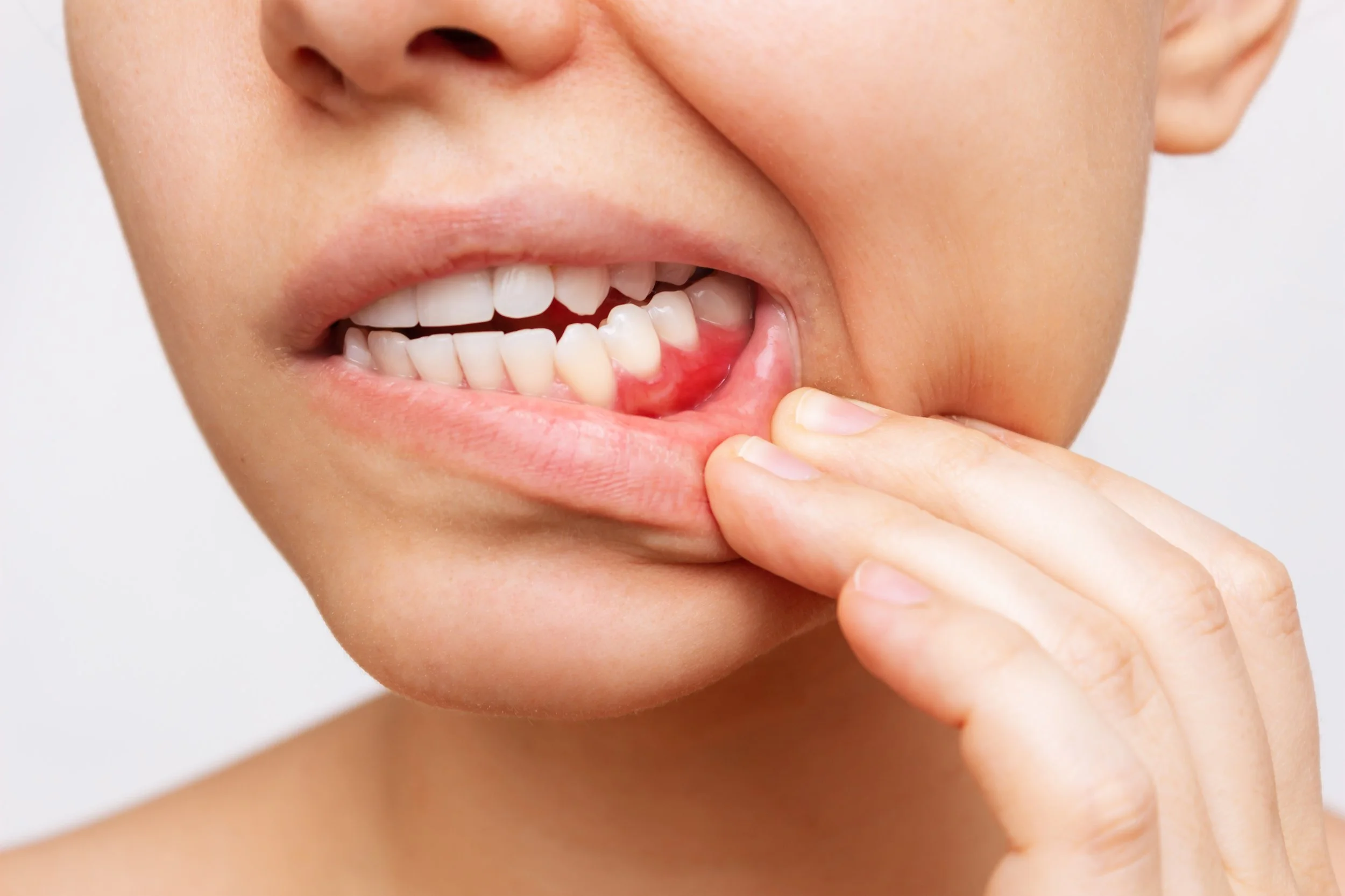
Red, swollen, or tender gums
Bleeding when brushing, flossing, or eating hard foods
Persistent bad breath (halitosis) that doesn’t resolve with brushing
An unpleasant taste in your mouth
Visible Changes
As disease progresses, you may notice:
Receding gums—teeth appear longer as gum tissue pulls back
Puffy gums that look shiny or inflamed
A visible dark line of plaque or tartar along the gumline
Exposed root surfaces that weren’t visible before
Advanced Signs
More serious symptoms of gum disease include:
Loose or sensitive teeth
Teeth that shift position or new gaps appearing between teeth
Changes in how your teeth fit together when biting
Painful chewing
Pus discharge along the gumline
Recurrent gum abscesses
When to See a Dentist Promptly
Contact a dental professional if you experience:
Bleeding gums persisting more than one week despite improved brushing
Sudden tooth mobility or loose teeth
Swelling in gums, jaw, or face
Pain around teeth or in the jaw
Fever accompanying oral symptoms
Don’t wait for pain to seek care. By the time periodontal disease causes significant discomfort, substantial damage has often already occurred.
A Note About Children and Teens
While advanced gum disease is less common in young people, gingivitis affects many children and adolescents. Persistent bad breath and gums that bleed easily—especially during puberty or in kids with orthodontic devices—warrant evaluation by a dental professional.
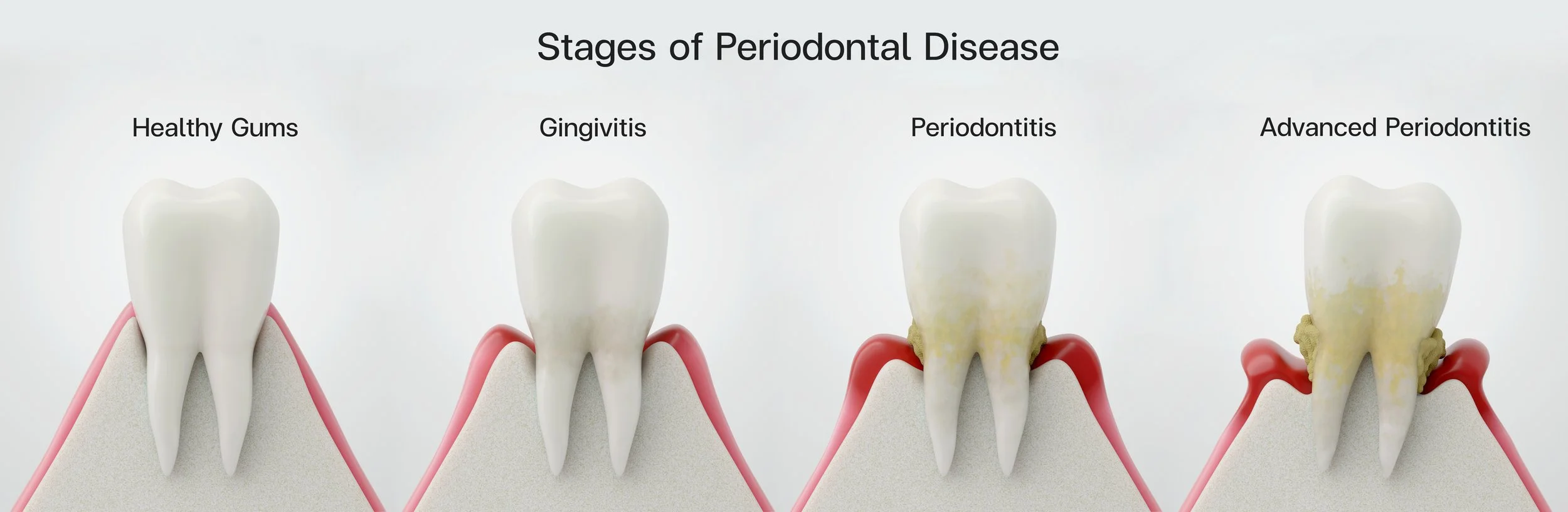
Stages of Periodontal Disease
Periodontal disease typically progresses through distinct stages, from reversible inflammation to increasingly severe bone destruction. The 2017 classification system adopted by the American Academy of Periodontology defines these stages based on severity, extent, and complexity of disease.
Stage 1: Gingivitis
Gingivitis is the mildest form of gum disease. Gums may appear red, swollen, and bleed when brushed. However, the supporting bone and deeper structures remain intact. With professional cleaning and improved home care, damage at this stage is completely reversible.
Key characteristics:
No bone loss visible on X-rays
Pocket depths less than 3mm
No attachment loss between teeth and gums
Stage 2: Early Periodontitis
When gingivitis is left untreated, it can progress to early periodontitis. Plaque extends below the gumline, and shallow periodontal pockets (around 4mm) begin to form. Early bone loss—typically less than 15-33%—may be detectable on dental X-rays.
At this stage of gum disease, you might notice:
Increased bleeding on probing
Mild gum recession
Occasional sensitivity
Stage 3: Moderate Periodontitis
Moderate periodontitis involves deeper pockets (5-7mm), more significant bone loss, and possible tooth mobility. Gum recession becomes more noticeable, and cleaning these areas effectively becomes difficult even with proper technique.
Patients at this stage often report:
Teeth feeling different when chewing
Visible changes in gum contours
Increased sensitivity to hot and cold
Stage 4: Advanced Periodontitis
Advanced periodontitis represents severe disease. Bone loss extends beyond the mid-root level, pockets exceed 7mm, and multiple teeth may be affected. Furcation involvement (bone loss between roots of multi-rooted teeth) is common. Patients may lose teeth or require extractions.
Signs of advanced gum disease include:
Loose teeth that drift or shift position
Significant gum recession exposing root surfaces
Deep periodontal pockets with possible pus discharge
Difficulty chewing or changes in bite
Variable Progression
Not everyone progresses through these stages at the same rate. Some individuals remain stable for years with good care, while others deteriorate rapidly. Factors like smoking, uncontrolled diabetes, genetics, and immune function all influence progression speed.
Regardless of stage, treatment goals remain consistent: control infection, stop progression, preserve supporting bone, and maintain as many natural teeth as possible
Treatment Options for Periodontal Disease
Treatment for periodontal disease is tailored to severity. Early-stage disease may require only professional treatment and improved home care, while advanced periodontitis often necessitates surgical intervention.
Non-Surgical Treatments
Professional Dental Cleaning (Prophylaxis)
For patients with gingivitis, a professional cleaning removes plaque and tartar above the gumline. Your dental hygienist will also polish tooth surfaces and provide instruction on proper brushing and flossing techniques. Regular dental visits for prophylaxis help prevent gum disease from developing or progressing.
Scaling and Root Planing (Deep Cleaning)
Scaling and root planing is the cornerstone of nonsurgical treatment for periodontitis. Performed under local anesthesia, this procedure involves:
Scaling: Removing plaque and tartar from tooth surfaces above and below the gumline
Root planing: Smoothing root surfaces to discourage bacterial recolonization and help gums reattach
Research, including Cochrane systematic review data, shows scaling and root planing produces significant reductions in probing depth and gum inflammation at 1-6 months post-treatment.
Antibacterial Approaches
Depending on disease severity, your dentist may recommend:
Localized antibiotics: Gels or chips placed directly into periodontal pockets
Antimicrobial mouthrinses (such as chlorhexidine)
Oral antibiotics for acute infections or aggressive disease
Surgical Treatments
For moderate to advanced periodontitis that doesn’t respond adequately to non-surgical therapy:
Pocket Reduction Surgery (Flap Surgery)
The periodontist lifts the gum tissue to access deep deposits of plaque and tartar. After thorough cleaning, bone may be reshaped if necessary, and gums are sutured at a level that reduces pocket depth and makes future cleaning more effective.
Regenerative Procedures
In select cases, regenerative techniques can partially rebuild lost supporting bone:
Bone graft using your own bone, donor bone, or synthetic materials
Guided tissue regeneration membranes that direct tissue growth
Biologic agents like platelet-rich fibrin to enhance healing
These procedures work best for specific defect types—particularly narrow, vertical bone defects rather than horizontal bone loss.
Soft Tissue Grafting
Gum grafting covers exposed root surfaces, reduces sensitivity, and improves gum thickness around teeth. Tissue may be taken from the roof of the mouth or donor sources.
Advanced Technologies
Some practices offer laser-assisted periodontal therapy, which uses targeted laser energy to remove plaque and diseased gum tissue with potentially shorter healing times.
Maintenance Therapy
After active treatment, ongoing periodontal maintenance is essential. This typically involves:
Professional cleanings every 3-4 months
Monitoring of pocket depths
Reinforcement of home care techniques
Assessment of risk factors
Treatment can control disease and stop progression, but success depends heavily on patient compliance with maintenance and home care.
How to Prevent Periodontal Disease
Most cases of gum disease are preventable—or at least controllable—through consistent daily habits and regular professional care.
Daily Brushing
Brush twice daily for at least two minutes using fluoride toothpaste. Use a soft-bristled manual or electric toothbrush with gentle circular motions, paying special attention to the gumline where plaque accumulates.
Interdental Cleaning
Floss once daily to remove plaque between teeth where brushes can’t reach. Alternatives include:
Interdental brushes (especially effective for larger gaps)
Water flossers
Soft picks
Regular Dental Checkups
Schedule regular dental checkups and professional cleanings at intervals your dentist recommends—typically every six months for low-risk patients, every 3-4 months for those with periodontal history or elevated risk.
Lifestyle Modifications
To prevent gum disease and support a healthy mouth:
Additional Habits
Replace your toothbrush every 3-4 months or when bristles fray
Wear a nightguard if you grind your teeth (bruxism can contribute to gum trauma)
Consider tongue cleaning to reduce overall bacterial load
The Connection Between Gum Health and Overall Health
Your mouth isn’t isolated from the rest of your body. Chronic gum inflammation can influence—and be influenced by—conditions throughout your system.
Cardiovascular Disease
Epidemiological studies show that moderate to severe periodontitis is associated with increased risk of heart attack and stroke. The proposed mechanisms include:
Systemic inflammation triggered by periodontal infection
Bacteria entering the bloodstream (bacteremia)
Effects of periodontal pathogens on blood vessel walls
Diabetes
The relationship between diabetes and periodontal disease is bidirectional. People with diabetes face 2-3 times higher risk of developing periodontitis. At the same time, severe gum disease can make blood sugar harder to control. Research from dental and craniofacial research institutions suggests that treating periodontal disease may modestly improve HbA1c levels in some diabetic patients.
Other Associations
Research has reported links between periodontitis and:
Rheumatoid arthritis
Adverse pregnancy outcomes (preterm birth, low birth weight)
Chronic respiratory diseases
Kidney disease
Cognitive decline and Alzheimer’s disease
Understanding Causation vs. Association
It’s important to note that association doesn’t prove causation. Confounding factors like smoking and socioeconomic status complicate interpretation. However, biological plausibility exists: inflammatory mediators and bacteria from the mouth can enter the bloodstream and trigger systemic responses.
The takeaway? View periodontal care as part of comprehensive health maintenance. Inform your dentist about your medical history, health conditions, and medications, and ensure your physician knows about any ongoing dental issues.
Is Periodontal Disease Curable?
This is one of the most common questions patients ask. The honest answer depends on the stage of disease.
Gingivitis: Fully Reversible
If caught early, gingivitis is curable. With professional cleaning, improved home care, and removal of plaque and tartar, gums can return to a healthy, non-bleeding state. No permanent damage occurs at this stage.
Periodontitis: Manageable, Not Curable
Once periodontitis has caused destruction of bone and attachment, the goal shifts from cure to control. Treatment aims to:
Eliminate active infection
Stop disease progression
Preserve remaining supporting structures
Maintain function and comfort
Limitations of Regeneration
Regenerative procedures can partially rebuild bone and ligament in selected areas—particularly narrow vertical defects. However, full restoration of the periodontium is rare. Horizontal bone loss and established gum recession cannot be completely reversed.
Patient factors significantly influence outcomes:
Smokers respond less favorably to treatment
Poorly controlled diabetics heal more slowly
Genetic susceptibility affects immune response to bacteria
Long-Term Management
Periodontitis becomes a chronic condition requiring ongoing attention. With consistent professional care, daily plaque control, and management of risk factors, many patients keep their teeth healthy for decades despite a periodontal diagnosis.
The key is commitment. Patients who attend regular maintenance appointments, follow home care instructions, and address systemic diseases like diabetes maintain stability far better than those who treat periodontal therapy as a one-time fix.
Conclusion
Periodontal disease is a common infection of the gums and supporting structures of the teeth, affecting nearly half of American adults over 30. Despite its prevalence, most cases are preventable—or at least controllable—with consistent oral hygiene and professional care.
Early detection makes all the difference. Gingivitis, treated early, is fully reversible. Advanced periodontitis, while not curable, can be managed effectively to preserve your natural teeth and prevent tooth loss.
Pay attention to warning signs: bleeding gums, bad breath that won’t go away, receding gums, or loose teeth. Schedule regular dental visits even when nothing hurts—silent progression is one of this disease’s most dangerous features.
Your oral health is connected to your overall wellbeing. By maintaining good oral hygiene habits, seeing your dental professional regularly, quitting tobacco, and managing health problems like diabetes, you protect far more than just your smile. Start today with the basics—brush twice daily, floss once daily, and schedule that dental checkup you’ve been putting off. Your future self will thank you.